Barriers to Feeding Young Children Well During and After Illness: Insight from the DRC
Written by: Madeline Kau, Emily Zimmerman (ideas42), and Augustin Ngandu (SBC Advisor, Breakthrough ACTION DRC)
For young children experiencing an illness, adequate nutrition is critical for recovery. However, children often do not receive the recommended amounts of food during and after an illness. In the Democratic Republic of the Congo (DRC), 70% of children under five receive less food than usual or no food during episodes of diarrhea. Similar gaps exist across many low- and middle-income countries like Pakistan (63%), Ethiopia (65%), and Peru (72%). In settings like these where childhood illness is common, too little food during and after illness contributes to high rates of child malnutrition, as children are unable to regain lost weight. Malnutrition, in turn, can lead to stunted growth and development and higher child mortality.
Why are young children not fed enough during and after illness? In collaboration with the USAID Advancing Nutrition project, Breakthrough ACTION conducted qualitative research with families and health workers in the DRC using a behavioral economics approach to answer this question. We learned that while caregivers want to feed their baby well, they understandably feel discouraged and at times powerless in the face of the myriad constraints they encounter. These significant constraints discussed below obscure steps that caregivers could take with the resources available to them.
Mental models of “worthwhile” foods limit the choice set
First, caregivers described a need for the child to recuperate strength lost during illness with specific, “high quality” foods they associate with strength, like meat, dairy, and eggs. However, most families can rarely afford or access these foods. Health providers reinforce this perception by counseling on the foods that are emphasized in their training and job aids but are often not available to families. A rigid mental model of “worthwhile” foods leads caregivers to underestimate the value of additional calories from simply feeding the child greater quantities of readily available foods. Redirecting attention toward locally available, affordable options such as small fish, fruits, and vegetables will expand a family’s choice set of which foods are worthwhile and may increase feeding during recuperation.
Strengthening coaxing skills can help overcome a child’s limited appetite
Second, caregivers expressed frustration with their child’s limited appetite during illness, which they saw as outside their control and a reason not to offer more food. Coaxing is critical for encouraging a sick child to eat, yet caregivers do not have broad repertoires of coaxing tactics. The tactic caregivers most frequently mentioned was offering their child’s favorite foods, but these foods are often unaffordable. Strengthening caregivers’ coaxing skills through counseling programs, workshops, or peer-to-peer sharing networks could empower caregivers to feel that they can win over their child’s appetite and allow them to feed more when the child is sick.
These insights and others identified through the formative research provide a roadmap for program design that supports caregivers to feed their children well with the resources they have, building skills and habits that are critically important during periods of illness and recovery but that remain relevant in times of good health.
Breakthrough ACTION and USAID Advancing Nutrition are currently developing a suite of solutions with caregivers and health workers works across multiple health system touchpoints to help families better feed their children to promote recovery from illness, fight off future illness, and ensure infants grow into healthy children and adults. Stay tuned for our full suite of solutions and more insights from our work supporting caregivers to feed their children well.

The consultation room at a health center in Sud Kivu, DRC. Providers and caregivers alike focus intensely on medical treatment during a sick child consultation and do not currently discuss lost nourishment. Optimal feeding during and after illness is a critical behavior not widely practiced. (Photo credit: Raissa Rwizibuka)

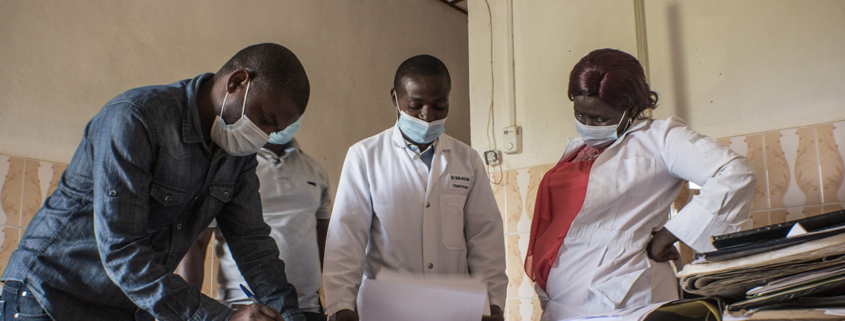
Health providers in Sud Kivu, DRC, give feedback on potential interventions to improve feeding of young children during and after illness. Photo credit: Raissa Rwizibuka

Sud Kivu is the region in the DRC where Breakthrough ACTION and Advancing Nutrition conducted research to better understand the barriers to feeding young children during and after an illness. (Photo credit: Augustin Ngandu)

 Raissa Rwizibuka
Raissa Rwizibuka Sara Holbak/VectorWorks/Photoshare
Sara Holbak/VectorWorks/Photoshare

 2019 CORE Group Global Health Practitioner Conference
2019 CORE Group Global Health Practitioner Conference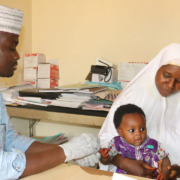 Breakthrough ACTION
Breakthrough ACTION Photo credit: amy Rakotoniaina/PMI/Flickr
Photo credit: amy Rakotoniaina/PMI/Flickr